The morning looks busy to me, but for that group I would say it's an ordinary and routine day. I arrive precisely at a time when I witness an exchange of teams, some are leaving, others are starting. The room is small for all the fuss, there is no wasted time there. There are two computers, always occupied by doctors who fill in information several times. There is a certain good mood, something mixed with the tiredness of someone who has just finished the shift and is about to go home. They talk about the coffee capsules one of them brought to share, some grab the lunch boxes now empty as they are about to leave, others just want to wake up better to start the long day.
I make myself comfortable in the room, afraid to appear intrusive, but no one sees me as such. Quite the contrary.
I listen to topics that make me slide a little more down the chair, just because of the feeling of fear that overwhelms me, while I fan myself with sheets full of tables that were, after all, being sought by one of the team members. Among the words spoken, I pick up concepts that are slightly familiar to me: they are waiting for the results of a biopsy, they are waiting for more details about an endoscopy and they are contacting another hospital to finalize data on the rescue of a patient who needs the care of these teams in Santa Maria. The doctors are coming in and out, almost all of them say “good morning” nicely. I arrived late, because what seemed to me an obvious and easy path, made me get lost again at Santa Maria Hospital. As such, I left Professor Susana Fernandes waiting for me, as if time was not important, but I know well how rare and precious it is to everyone's agenda. My absolute embarrassment, but I quickly settle there. I I feel like coming back over and over again.
Susana Fernandes is an Intensivist in Santa Maria Hospital, responsible for Medicine II, Intensive Medicine Coordinator and Director of the University Clinic of Intensive Medicine of the Faculty of Medicine of the University of Lisbon. She is asked questions by the various teams every minute. They are used to checking whether it is really essential to speak at that moment, or whether it can be done later. We're going to talk about the dozens of students who volunteered to support the Intensive Care Medicine teams. In a few minutes, she will resume one of her routines interrupted during the peak of the pandemic, teaching classes, now via zoom.
I take notice of some names and faces. Ana Rita, Hospital Assistant in Internal Medicine and training in intensive care medicine, and João Oliveira, year 3 intern in Nephrology and with whom I speak between interviews that take place there throughout the morning. I say good morning to Pedro, another doctor who comes in. I chose to join the good spirits and reinforce the “welcome to another day of work at our Hospital”. The idea seems to be well received, who doesn't like to be treated cheerfully?
These people, all with an empathetic face, tell me about a special patient who for 92 days ago (at the date I wrote this article) almost breaks down and says goodbye to life, but almost every day gets up and informs that it is not his time to die yet, because he does not want it that way.

I spent the morning at the Intensive Care Medicine Unit, after a brief meeting with one of its members, Dr Nuno Gaibino, a FMUL former student and someone who has always maintained emotional ties to his Faculty and its people. He told me that 130 students had been through the Covid Intensive Care Medicine wards because they wanted to help, even if it was risky for them. Over a few months and after a long period of exhaustion, Santa Maria Hospital opened its most private doors to medical students and asked them for help in taking care of patients infected with SARS-CoV-2.
The embryonic idea arose in mid-November, when the Intensive Care Medicine Unit, Covid area, was overworked. There was the sensitivity to accept outside help and some ideas were even exchanged in this regard. In January, the Director of Intensive Care Medicine, João Ribeiro, returned to the subject, claiming urgency in its enforcement. Quickly, what was just an intention, became practice. Coordinated with the Student Association (AEFML), and in agreement with the Faculty's Board of Directors, the plan to involve volunteer students, from between years 4 and 6, in Intensive Care Medicine was implemented.
There were not enough pairs of hands, and the team in charge of the 7 Units that provided care to patients infected by SARS-CoV-2 was the same. Susana Fernandes gave me the calm and thoughtful report. After all, those who work in Intensive Care Medicine have these characteristics already innate to her. "We needed help for some moments of less differentiated work, but that required knowledge of clinical lexicon, which students from the upper years would know how to master.
We ascertained how many students might be interested and I admit that, against some of my expectations, around 130 to 150 students applied. There were many! And so we tried to make the most of their desire to help, even because we recognized that there could be some pedagogical aspect to add to their academic life. We tried to really involve everyone. With this in mind, we created the greatest number of shifts and rotativity that would allow them to come more than once, for one or two consecutive weeks for each student, a total of four days each. The truth is that as of March, there was less need for support, because the number of hospitalized patients also reduced significantly. If on the one hand, they came to help, on the other they also came to complete their clinical contact, thus reinforcing a side that was underprovided due to the pandemic”.
What tasks could they take on?
Susana Fernandes: They monitored the patients a lot. Many patients were sedated and when they wake up, they are confused and need to have someone close by to communicate with them, keeping them company and providing some integration. They collaborated with us in positioning the patients, because it was necessary to place them in the prone position (when the patient is lying face down on the abdomen, with the head turned to one side). They became involved in activities close to the patients, to help us use techniques. They also helped with registration tasks, because our ability to do them wasn't effective, we weren't able to do everything, even because we kept the research strands in the Covid area.
How was the reaction of our students to these real scenarios?
Susana Fernandes: Mainly great enthusiasm. But there was all sorts of reaction, some fainting episodes, but short-lived. The following day they came back and wanted to start all over again. The truth is that the atmosphere was harsh, not only because of what they saw, but because they were much more dressed. But they all adapted very well. And from a civic point of view, it was also very important, many of them felt they were far from reality. I even talked about this topic with António Velha (President of the AEFML). For these students, if they hadn't collaborated or watched anything in this pandemic phase, what would they remember in 5 years' time when they looked back? They really wanted to get involved in these activities and did so on other fronts, such as the Saúde 24 line and other types of solidarity actions. But this was, without a doubt, the real ground.
And for you, the medical team, was it important to be in contact with a possibly more naïve group, less tired and pressured?
Susana Fernandes: They brought different energy... I remember that for one of the students, just wearing the PPE gave her such enthusiasm that she photographed everything, after going inside and contacting patients, She was totally happy. There were others who spent more than two hours talking to a patient, then came back to keep up with their follow-up process. We had two or three cases of people who came to help and who really wanted to do it, but asked not to go to the Covid area, they did the most bureaucratic part. But the vast majority really wanted to go to the Covid area and wanted to be there at the patients’ bedside. They helped and accompanied the nurses a lot and that was very enriching for them.

How was the management of human resources in Intensive Care Medicine, whose number of patients doubled in size, but not the team? How did you manage it?
Susana Fernandes: It was... (she hesitates, thoughtful). It required great dedication and great resilience. That's essentially what got us through. Then we were much more divided, we usually work as a team, made up of seniors and others who are more junior. And here we all had to separate ourselves, each senior was left alone to receive the collaboration of other doctors who came to us from the most diverse areas.
During this period, were you never able to stop and rest?
Susana Fernandes: No... In the space of a year, only now are the first holidays being taken. But we managed to get here! And we're teaching here in Intensive Care Medicine again, something that had to stop because we didn't have any capacity. Professor Catarina Mota (also from Medicine II) and I have already gone back to teaching, there was a time in January and February when this was unthinkable. Fortunately that period coincided with the time of exams, when it became impossible to have classes at all. From March onwards, everything got better again.
What do you foresee in the next few months, given that we are already experiencing a very generalized lifting of the lockdown?
Susana Fernandes: It's difficult to make this prediction, because even in January there were several explanations for what happened and there wasn't only one possible reason. Therefore, everything will depend a lot on the capacity for mass vaccination in the coming months, this will be the most important step. Then it is important to understand the strain of the virus that is circulating. I personally believe, and I am not an epidemiologist, that we will not go back to what happened in January. But if another third wave came, it would be extremely complicated, because the teams are exhausted.
It is important to mention that the year 6 students, at the request of Professor Helena Cortez Pinto, were diluted between areas because they had little to do and did not know how to act, where to go. We alone had 5 students here, and it was a very enriching contribution for us. So much so that we really want year 6 students to become integrated into our teams. They can acquire excellent knowledge and thus take a qualitative leap in their path. I can tell you that their commitment was such that in the end they could be compared to the younger interns. This happened in the scope of the pedagogical internship, which made them obtain a final grade.
Would it make sense to involve, in a cyclical and continuous way, students, from year 4 onwards, enabling them to have an increasingly closer approach to reality?
Susana Fernandes: This idea is valid, but it is more complex than we might think. For them to come to a Unit, it is also necessary to create the right circumstances for them to adapt and learn. And we have to be available to explain and accompany them. It would be necessary to prepare the students themselves in advance. They would have to understand which behaviours are appropriate with patients, understand the patients’ space. It would need organized training, as we did to receive these volunteer students. But the experience and contact with the clinical reality are very interesting, even for them to know exactly what they want to do, and why they have contributed to the services.

The medical student volunteering project continues, but of the 7 Units that were active at the peak of the pandemic, there are now 4 areas in operation. The good news is that it is no longer urgent to have extra support from these students, not because they don't want to continue giving it, but because the rate of reduction in infected people has dropped on a large scale.
Final testimonials were requested from this group of volunteers. It is confirmed that the mass adhesion also gave them strong motivation.
It's worth getting to know them!
Romana Rodrigues

Year 6 student – It wasn't because she was in year 6 grade that she didn't volunteer. The truth is that her internship in Internal Medicine was on hold due to the pandemic and going to the Covid ward was her challenging alternative.
Mother of an 11 month old baby, she now has to study for the National Access Test. A few weeks ago, Romana entered the Hospital at 9 am. Her first task was to check on the patients who, each day, could change. She refers with great appreciation to Susana Fernandes, who allocated one patient to each year 6 student, always under supervision, but with an equal vote of confidence. Before she went to see her patient for the day, the steps remained the same: read the person's medical record and only then get equipped with the Covid suit (PPE) and enter the restricted area. Departure times, which should have been lunchtime, always ended up being later. For two intense months, she fell in love with Intensive Care Medicine and the adrenaline it causes. Were it not for motherhood and the responsibility it implies, Romana would have chosen this area as her final specialty without hesitation. But being a little older than the average of her peers and due to her current life, she will remain faithful to her first great love since she chose Medicine, Gastroenterology.
"I knew there were risks in coming to this area, because we weren't vaccinated. I was afraid if we would have enough knowledge to be able to help. But between taking risks and being able to seize the opportunity, I didn't hesitate. It was something so enriching as it was frightening, particularly in the first week. I felt that I needed subtitles for everything, everything was said in acronyms and until now we had only heard them in some theoretical classes. In this area, we are faced with the reality of having to work with organ support and we weren't exactly prepared for it. It was a race against time, I knew that as a student, I had to help, but without delaying the dynamics of those who were already here. When I got home I read several articles. When I thought I knew something, I arrived at the Hospital only to realize that everything was totally different. In fact, when we study, there's the ideal setting, in a controlled environment, and then there's the hospital and real life. The applicability of what I read was not so clearly evident afterwards. Of course, I had a lot of difficulty, but facing doubts and difficulties is part of the routine of a year 6 student. There is a story in particular that I'm going to take from one of the patients who marked this entire medical and nursing team, and which reflects the resilience of humans. We learned that being fit and healthy, pre-covid, does not mean that you will not always be unscathed when it comes to health, because it is something wrong. We then learn to believe a lot in human strength, because almost daily there is a patient who absorbs a negative impact of the disease and gets back on his feet and always wants to wake up the next day. Being here in this Service gave me a notion of the medical dimension, but also of the human and his inner will".
Margarida Sá Machado

She is from Braga and is in year 6 of the IMDM. She always looked at year 6 students as people who knew a lot, and every year she completed one year of the degree, she aspired to reach that stage. Now a final year student, and faced with a pandemic that has changed the rules for everyone, she thinks year 6 students are closer to the inability of a child than to the wisdom of the solution of a grown-up. She shows her humility, now that she knows that "the more she knows, she realises that she knows nothing". She reflects about the equal treatment between doctors and students, and thanks this fact for the non-hierarchical relationship among peers, something that was unthinkable along the academic path. She did all her internships in Santa Maria, in paediatric surgery, then general surgery, but the latter felt next to nothing, because it was only two weeks, when in a normal phase it would be six weeks of mandatory internships. She always liked the dynamics of Intensive care. For Margarida, intensivists are the "most complete doctors". January arrived and Margarida was involved in the Hospital's reorganization of the 15 patients at the ward. At that time, Margarida was doing a curricular internship, the only certainty she had is that one never knows what the next day would be like. She remembers her last day of conventional internship, it was the day she helped to transfer those 15 patients to Pulido Valente's infirmary. Her internship area in Santa Maria was now just in the Covid area. After the internship ended abruptly, due to the inability to keep the students and because there was a serious risk of contagion, they went home not knowing what to expect.
It was at that time that she became aware of the opening of vacancies for curricular internships for year 6, and she was one of the first to become involved. She forgot, however, to inform that she was facing a pyelonephritis (bacterial infection of the kidney), devaluing the fever and the pain and total weakness she felt. Wearing a PPE and spending several hours with breathing confined to a closed suit and mask caused her several fainting feelings, but she never gave up. For months she avoided her family for safety and controlled her homesickness for those who are her safe haven, but admits that now that she has returned home, she has needed a lot of comfort. In this last year she realized that she should not be ashamed to ask for comfort and support, because emotion or vulnerability do not mean weakness in a student who is always being prepared not to fail. And will it be without weaknesses that Margarida wants to be in life as a doctor? It's clear to her that she does not.

"In the Intensive Care Medicine Covid I felt much less fear than in a normal ward, because every day we only had access to surgical masks and a disposable suit. Every day someone came from the secretariat to say that “one more contact had come up in the ward and there was a new person infected.” We were tested immediately, but there was not always time to be sure of the results of these tests. It was a big daily uncertainty, because nobody knew where the risk came from. And in Intensive Care Medicine, from the moment we enter the Covid Unit, we know that we are protected from head to toe and there was nothing else to do to safeguard our safety. Of course the first procedures are imposing.
It was enough to leave part of the hair visible for risk of contagion. At this stage, I felt that we have a generation that is very attentive to each other, that knows that a hug is sometimes enough for someone to gain strength. Just to be next to someone who comes out of a ventilator and give a word of encouragement. People are scared, being surrounded by machines and noise is scary, these patients are scared and often wake up connected to the ECMO. When these same patients fell asleep, they didn't know what was going to happen to them. It's like waking up in a nightmare, even though the ECMO is the machine that will save their lives. These patients trust us with their lives and sometimes they knew they would not survive. Still, they were grateful that we took care of them to the end. This learning is worth much more than a good grade, a good grade can blind us and Medicine has a magic far beyond that. Only in contact with the Services we know what reality is. Maybe I didn't study as much as I should for the exam that will take place in November, but what I learned in clinical practice gives me priceless baggage".
Note - Margarida submitted her thesis on 10 May and the viva voce examination will be on 28 June. We wish her all the best!
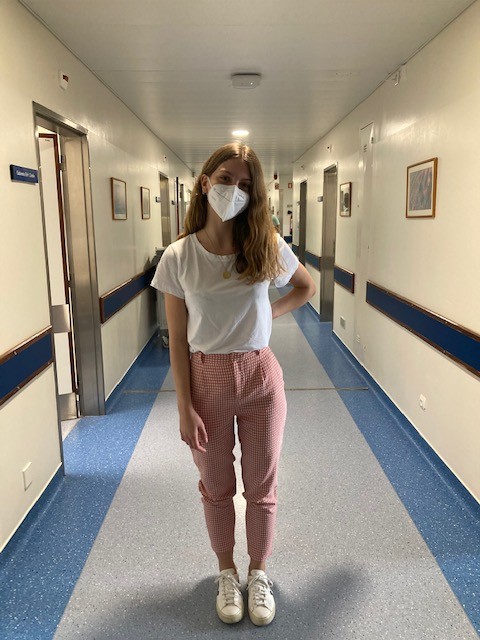
Joana Asseiro
Student of year 4 of the IMDM, she volunteered after spending the 2nd semester of her year 3 on hold and not knowing what academic life would be like. Enrolled and accepted, Joana regrets that she "she only managed to attend two mornings at the Covid infirmary". She came on a Saturday and stayed until Sunday. Her elder sister is going further along the path of becoming a doctor, she is an anaesthesiologist in Coimbra, birthplace of both. Joana knows how to see the positive side of life, even when she is aware that there is a flip side. These times have shown it, but that doesn't mean she looks at her surroundings with less magic. Distance learning classes? She could have faced a problem, but she preferred to see the solution. The transition from physical to virtual came to benefit her, she explains, allowing her to review classes and improve grades and notes. But it was necessary to strengthen the practice and start training in the preparation of the clinical history, in making the objective examination of the patient, as well as in semiology manoeuvres. Joana found herself "trapped in herself", however she did not resign herself to the forced decisions of circumstances and decided to offer her hands for a greater work.
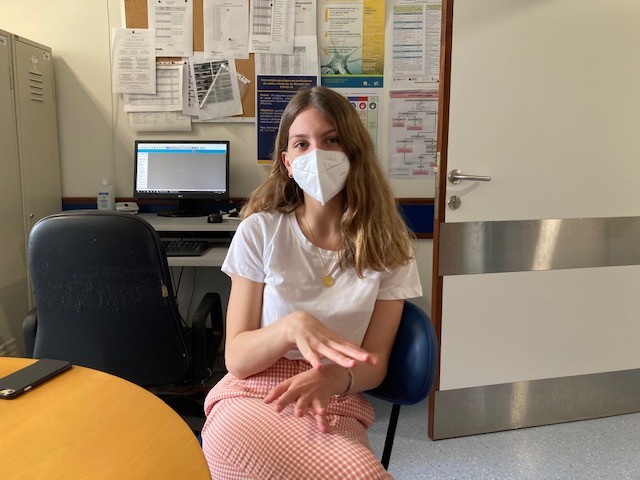
"Each person does what he or she wants from the Medicine degree, in the sense that it is up to each student to find ways to gain more experience and contact with reality and with the clinical component. We need to move, do things, we must insist on getting involved in all the procedures, and that brings results, it works. I always tried to have more practice, as the degree prepares us a lot in theoretical terms. Of course, we manage to adapt and, as we do the specialty, we acquire more experience, but it's hard for me to wait for that to happen. I really like going to the wards and gaining experience. When I signed up as a volunteer, my fear was that I would be useless, that I wouldn't know how to do anything. On the other hand, I thought that was the best way to learn. We have to learn to solve our problems. It is only hard the first time, which is horrible, then you just keep trying. When I arrived at the Covid Ward, I felt fear, I admit it, I read and reread the email they sent us explaining all the steps. As soon as I arrived, I was received by Dr Nuno Gaibino. He and the interns were tireless, showed everything, explained everything with the greatest care. By the time I arrived, there were no patients with active infection, so I didn't even have to wear the PPE. I actually felt sorry for myself, I wanted to experience that part, because I was living it very intensely. But it was already March and luckily there were almost no infections. I went with a team to see patients and, of course, we used proper protection, like FFP2 masks, gloves and always disinfecting everything. The focus was to see patients who had already been infected and had great muscle deficit. When they are bedridden for a long time, they lose mass and there is an atrophy that is characteristic of these Intensive Care patients. I had never been to an ICU and had no notion of human weakness. We are never prepared to see everything and I came precisely with the intention of understanding if I had the structure to work in such an area or not. I admit that when I left I thought I didn't really want to go down this path, it's too hard for me, but it was great to come to know how to draw my own conclusions".
Gabriela Rodrigues


She is in year 4 of the IMDM and has dual nationality, part of the family is from Floripa and Gabriela keeps counting the weeks to go back to one of the places in her heart, Brazil. She started as a volunteer in Intensive Care Medicine at a calmer stage. The truth is, she wanted to get in on the first shift, to get into the chaos. "Whoever is in Medicine wants to help", she explains as a logical condition for those who reached the first year that would provide them with a connection to the clinical component. She was looking forward to the experience, but the academic course came to a halt without being able to control anything. Unmotivated, because times had forced her to slow down, it was clear to her that she was far from putting her best self into the things she did. It was as if she wanted to go further, but she lacked the real momentum, the opportunity. The scenario of some despondency would change from the moment she was told that she would join the Intensive Care Medicine teams, as a volunteer in the Covid area.
"The first encounter was not easy, like a young fish in an ocean too big for its size. New lexicon, new rhythm between doctors and patients, all this gave Gabriela a feeling of being “too small” for such a challenge. But she took advantage of the opportunity to show why she wanted to be there. It didn't start small, one of her first contacts was a patient at the ECMO. She stayed for a weekend and, after Easter, she came back for another period of time and gained her real present, the lady who had been connected to an ECMO was out of danger. She had never seen anyone so fragile in front of her, seeing the scenario of fragility in the news was usual for her, but in front of her eyes it was too hard a clash. Still living with her parents and sister, she did not ask for their opinion regarding the decision she made. Mainly concerned with the health and well-being of her parents, she just warned: "Mother and father, I'm going to the Intensive Care Medicine". So it was.
"The people I met were highly debilitated. They were young, just over 50 years old. This moves us and what we had as conviction. And it shows that what I had seen in the news was real, everything the same. I spoke to my Professor Nuno Gaibino and this was the scenario they lived through, to the limit”.
Katerina Drakos

She is in year 5 and has always been involved in numerous academic projects and solidarity causes. Director of Clinical Exchanges for Incoming students at ANEM, she first learned to speak English, only later learned Portuguese, a logical path for someone with dual nationality and a father from Cyprus. The pandemic initially took her to the Saúde 24 line, where she provided information to callers asking for help. The shifts stopped as the turnout had diminished. She continued her life as a student until she received a new mail. Volunteering in Intensive Care was the help she wanted to give, in the face of a pandemic situation.
She managed to get in during the first few months, which allowed her to be at the infirmary for three weeks. She reports on starting immediately with patients in critical condition and almost all infected by Covid, managing to follow the evolution of patients and watching a ward no longer with so many critically ill patients due to infection.
She decided to read scientific articles because she wanted to master the lexicon she could not yet command. Welcomed by Nuno Gaibino, one of the doctors who was always welcoming all the students, she still had time to receive transversal information, to feel less out of place. Katerina's role was to maintain ties and communication with patients. The first few days she describes as a shock, she saw cases that will eventually accompany her forever in the memory of someone whose view of reality has changed.

"The day I started I saw an intubated lady. She couldn't even talk to us, but she was gesticulating and crying. When we called her family, she couldn't hide the anguish she felt at being there, in that degree of dependence and not being able to appease her own family. I felt like a mere spectator, I just held the phone and felt like an intruder. Me and a friend who also volunteered were feeling the same. By the second day, the lady had been extubated, which meant she was slightly better. And in the third day she was talking normally and was extremely nice. What seems strange is that by the third day we had already created a strong bond with her. We realized the impact that we also had on her when, after almost an hour of talking, we were going to leave to talk to another patient, and the lady asked us to stay. She asked for time with us, needed more attention. In the end, she thanked me a lot, said that it had been one of the most important moments in her life. Those sick people feel completely alone, connected to machines, with different tubes and surrounded by different noises all the time. Beyond that, they see few people and those they see they can only identify them by the eyes. Everything else is covered. It was funny how this lady told us we were beautiful and actually she only saw our eyes... There was another lady who really impressed me, she owned a bakery and, when the pandemic started, she started making chorizo filled bread for everyone in the medical teams and came to deliver it herself. She tried to help so many and ended up getting the disease. Luckily she was fine afterwards, but it seems almost unfair, doesn't it? I was lucky, because I fulfilled my objective of establishing social contact. But that had a lasting effect on me, because when we return home, those people do not disappear from our thoughts.
I'm usually a positive person and I realized that I've only just been faced with death, I've thought a lot about the process and it's so complex that I don't know how to talk about it yet. I took the afternoon shifts and walked home, it was already dark. I remember that I was listening to a podcast that referred, precisely, to the absence of human connection with patients and the inability to know nothing about the person's life story. That marked me a lot. And it also made me reflect on how in my first years of training, we were not given the best messages, because the patients were referred to according to the number on their beds. A patient is not just a bed number and about whom the medical record will be written. The patient is a person who has a history. There is still a lot to do with the human component and volunteering has taught me that. We need more of these experiences, with a voluntary and patient contact component. Because it's very different to learn about something, or to be in contact with something real"
Mariana Dores

Mariana Dores is in year 4 and joined Intensive Care Medicine in April, during a calmer phase. In her 1st year of the nursing internship, she went to the Paediatric Intensive Care Unit, a remarkable moment as she witnessed the death of a baby just six months old. For days she was terrified and couldn't go out with her friends, or simply sunbathe on the beach alone. The clash with reality appealed even more to her sense of humanism towards patients. So it is not in vain that she idealized a correct Medicine where all patients, from babies to the elderly, are esteemed and looked after with the greatest care, which means extreme care with hygiene and comfort. Going to the Intensive Care Medicine Unit was no less impactful, talking to patients whose communication only happened via the eyes was a new learning experience. What to say without hurting feelings? What kind of information can be given and what topics can be referred to for communication to be stimulating? These were some of her concerns. She has a special passion for Internal and Intensive Medicine. Going home and watching the world unfold without her intervention was too strong an impotence that honked in her ears that she wasn't helping anyone. She has known Nuno Gaibino since the days when he was Anatomy assistant at FMUL and it was with him that she began to get involved in the Emergency Room. Since year 1 of the IMDM, she has enjoyed contact with the clinical component, always putting that into practice, accompanying Nuno Gaibino in the Emergency Room and interacting closely with many of those who were also her Professors. She said that some of her Professors ended up training in Intensive Care Medicine, inspired by a moment as hard as the pandemic. They knew they had to act and be able to help new patients even more. With an adrenaline rush, Mariana acted quickly, since the most varied decompensation scenarios come into the Emergency Room and revert through effective medical actions. The sense of help is something that accompanies Mariana since she freely exercises her will. That's why instead of spending the holidays to rest, she prefers to do volunteer work with those who need care the most.
With Mariana, it becomes clear that a doctor also needs the patient's cooperation so that progress can take place, and this relationship becomes an unbreakable bond.
She admits that she probably lives in a utopian world, because she thinks the sick deserve to be taken care of and "spoiled". She believes that one should do everything for the sick. Soon when Mariana becomes a doctor, we will know that she will fight for each patient until the end. So, we can only wish to have more people like Mariana.

"The hospitals were collapsing and I was at home. It was horrible to see this scenario and that was all I was thinking about. I signed up as a volunteer for Intensive Care Medicine as soon as I could. I entered a unit where the patients had been connected to the ECMO for over 60 days. My contact was different, because these patients were already part of the "medical family", which means that when these people decompensate, the clinical team too, because they are all connected with each other. Medical teams suffer for these people. The greatest lesson that Intensive Care Medicine gave me was that what dominates a doctor and the team is patience, that is, today we may not have a result, nor tomorrow, nor many days in a row, and the result will only be a month from now. And it takes calm and patience to believe in the patient and just control the situation, without dictating sentences. Opposite to what I learned in the Emergency Room. Here in Intensive Care, we exercise, in fact, a lot of patience. The case I dealt with closely was a lady connected to the ECMO and unable to speak. The instructions I received were to stay with her and communicate, to keep her company. I spent three hours talking with her and it is different from what we are used to, because her feedback is moving her eyes, and also through silence. The patients are intubated and in the case of this lady, she will possibly have to undergo a lung transplant, because she no longer has respiratory function. In this case, one can only work the muscles, through respiratory physiotherapy. This work involves a lot of patience and belief in the patient. I was talking to this lady for two hours and I didn't get any reaction or response. Two and a half hours later, she began to react and respond, moving her eyes. Now I understand why they called us at such a critical time, because the doctors didn't have time for everything and it's very important to interact with the patients. Stimuli can help a lot in the evolution of the clinical condition”.
Final note - to this entire team, thank you for the incredible generosity and the available way in which you welcomed us. This includes all those not referred to directly in this article, but who we praise.
Joana Sousa
Editorial Team


