“The disease has always afflicted human beings, because the disease is inherent to life: and man always strives to face this reality in the best possible way”.
(George Rosen, 1910-1977)
Throughout the world, drugs used until the end of the 18th century had the sole objective of curing diseases.
When, in the late 18th century, British naturalist and physician Edward Jenner (1749-1823), today widely known as the "father of immunology", discovered a drug - the smallpox vaccine - the history of drugs took a giant step. The purpose of this new medicine was not to cure, but to prevent, seeking to stop people from becoming infected by that disease, which would certainly lead to death. After this discovery, drug therapy also became preventive.

Smallpox, considered a serious public health problem, was an infectious disease caused by the orthopoxvirus, one of the largest viruses that infected humans. There have been countless smallpox epidemics described throughout history, which have travelled across continents and wiped out vast populations.

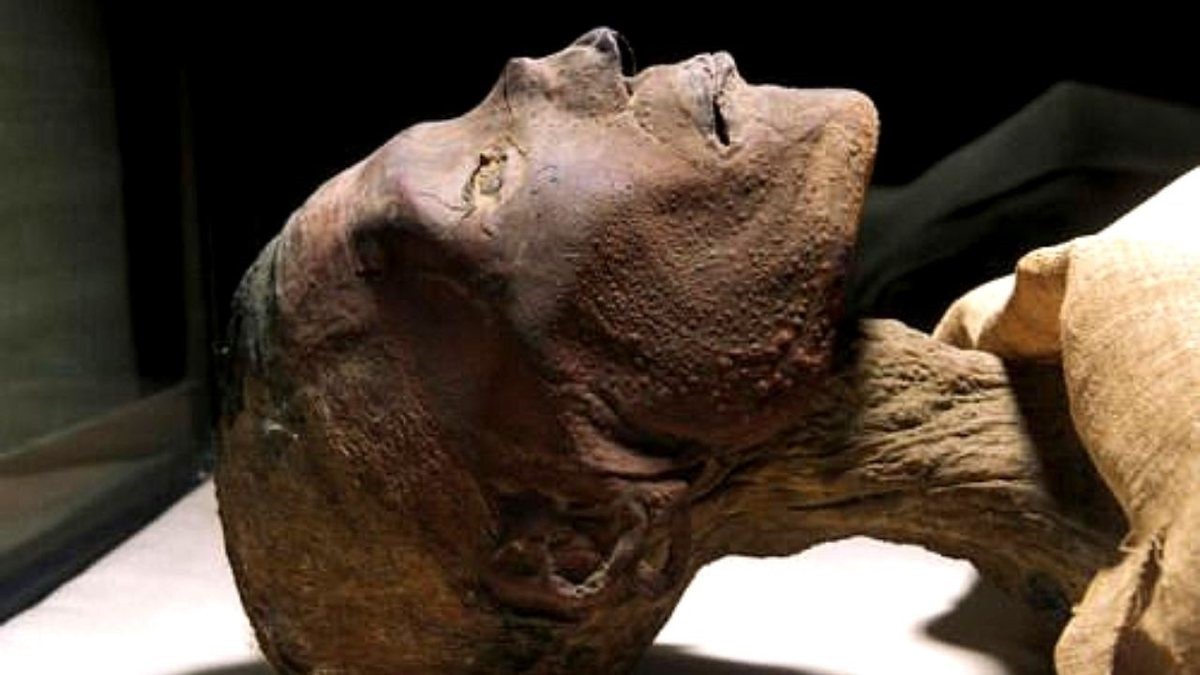
According to many research works, the oldest vestige of smallpox dates back to the Pharaonic era, as seen in the image of Ramses V, who lived three thousand years ago, which shows marks of the pustules on the head area. This disease also affected the Roman Empire and the American continent, after the arrival of Columbus in 1492. Documentation written in the 4th century, originating in China, refers to descriptions about symptoms of this disease.
It is believed that it was in India and China, over a thousand years ago, that the first attempts were made to immunize children against various diseases through a small cut on the arm, rubbing the scabs of infected wounds or other materials infected with smallpox in the wound. So, despite not understanding the explanation, the truth is that they created a response in the immune system and created immunity to the disease.
The method called de-variolation was also used in China, India and the Arabian Peninsula, although its origin is not well known. This practice arrived in Constantinople, brought by the Arabs or by the travellers who came from North Africa, and consisted of rubbing the dry scabs of smallpox that contained the virus, on the skin of the person to be immunized. The Chinese, for their part, grind the dry crusts to a powder, exposing them to hot steam, damaging the viral particles. The powder was blown into the nose of the person to be immunized.
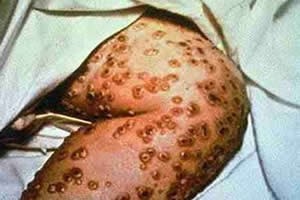
In Europe, for centuries, hundreds of thousands of people succumbed to this infectious disease every year, which corresponded to 30% of those infected. At first, the disease manifested itself through fever and vomiting, followed by rashes with pustules, filled with liquid and a hole in the middle, spreading throughout the body. After ten days, there was not an inch of skin free of blisters, which contributed to the fact that, after healing, patients who survived were disfigured, with terrible marks, which made them very vulnerable. One third of these victims went blind.
The most popular method of variolation used was inoculation, which was carried out using a smallpox sample obtained from a patient or a victim, which was injected into an individual subcutaneously with the help of a needle.
Around 1718, at a time when Europe was being affected by a strong smallpox epidemic, Lady Mary Montagu, wife of the then British ambassador to Constantinople, who had been infected with smallpox and her face had become very deformed, when she became aware of this practice decided to variolate the son in that city. When he returned to England, he made this practice known to his friends and members of the royal family, who also decided to undergo this method.

In 1721, Scottish surgeon Charles Maitland (c.1668-1748) carried out a variolation test on six prisoners. After being exposed to smallpox, everyone survived. Maitland also did this experience on two princesses from Wales, which made this practice fashionable in Europe. In colonial America, in Boston, Reverend Cotton Mather used this method on African slaves.
According to history, Catherine the Great, Empress of Russia (1729-1796), who was afraid that her son and herself would be infected with smallpox, (her husband, Peter III, who had been deposed and later murdered, had escaped the disease. However, he had marks on his face and head which caused him enormous instability), in 1768 called English doctor Thomas Dimsdale, who in the previous year had published the book The Present Method of Inoculation for the Small-pox.

This doctor, who had dedicated his entire life to the study of smallpox, exposed in his work the experiments he had carried out using that technique, which had been practiced for several centuries in India and China. This technique was characterized by removing material from the pustules of a sick person and applying it to the skin or nostrils of the person one wanted to protect.
As a rule, inoculated people, although they may show some symptoms such as fever and mild rashes, became immune to the disease. Dimsdale, when confronted with some deaths of people who had been inoculated, said in his work that "Those who died were always fewer in number than those who would eventually succumb to smallpox".
When Dimsdale left for Russia, he was afraid that his method would fail, because he knew that Empress Catherine did not admit mistakes and had no objection to having him killed. As it turned out, the English doctor left a cart next to the palace gates in order to escape, if his work was not satisfactory. The variolation of the empress and her son was a success. Thomas Dimsdale returned to England with the title of baron of the empire and with a lifetime pension, granted by the empress as recognition.

Variolation is not without risks, as variolated individuals could spread the virus and even die. However, the mortality rate was significantly lower (1/100) when a person acquired the virus from variolation, in contrast to when they were naturally infected (30/100). Variolated individuals also had a milder form of smallpox than those who had been infected by chance.
Around 1796, in China, after an outbreak of smallpox, those who survived were observed, and it was shown that they had been immune to relapse.
English doctor Edward Jenner, in the face of these events and after several years of observation study, found that when there were outbreaks of smallpox, there was a professional stratum that systematically did not get sick - the dairy farmers who milked the cows. On the other hand, he found that these people had a disease not as serious as smallpox called “cowpox”. Jenner wondered if people who were infected with cowpox, such as milkmaid Sarah Nelmes, were not infected with human smallpox, so he thought about contaminating some people with cowpox.
The first experiment carried out by Edward Jenner took place on 14 May 1796 on an 8-year-old child, James Phipps, the son of his gardener. He continued this experiment on other people, always with success. He had discovered the first vaccine. The word vaccine comes from the word vaccinae which means “from the cow”.
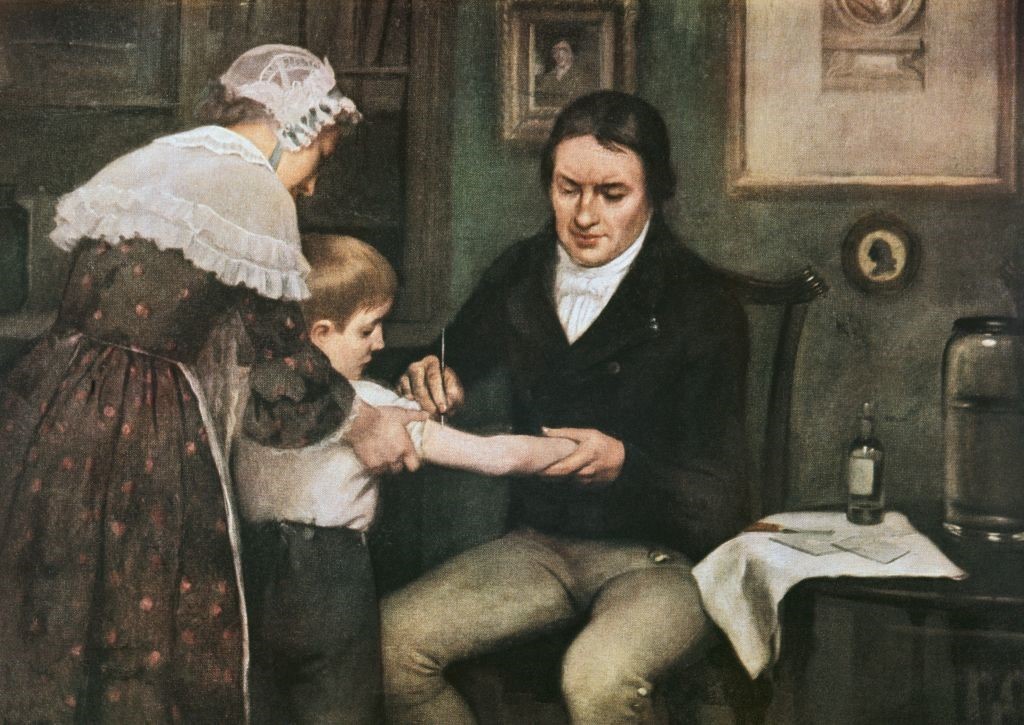
After realizing that his discovery would have profound benefits for everyone, Edward Jenner proposed a vaccine despite having no knowledge of immunology or of viruses and bacteria, and in the same year published his study An inquiry into the causes and effects of the Variolae Vaccinae, a disease discovered in some of the western counties of England, particularly Gloucestershire, and known by the name of the cow-pox.

However, Jenner was not the first to use this technique. Twenty-two years earlier, farmer Benjamin Jesty (1736-1816), having heard that dairy cows that caught cowpox were protected against smallpox, inoculated his family with liquid from the udder bubbles of infected cows - Jesty had already been affected by the bovine variant. In 1774, the English village of Yetminster was affected by the disease, and Jesty's family escaped the epidemic unscathed. In 2006, this achievement was recognized by the research support institution Wellcome Trust, which acquired an oil portrait of the farmer.

Smallpox did not choose social strata to make its victims. There were countless renowned people who died of this disease:



Some of the individuals who were only infected with smallpox:



Throughout history, there were several methods and experiments carried out until reaching what we know today as a vaccine. However, Edward Jenner is credited with the vaccination due to the scientific rigor with which this English physician supported his experiments.
Vaccination to combat smallpox started in 1796. Unlike variolation, which used the smallpox virus, the vaccine followed Jenner's example of using the less dangerous cowpox virus to create immunity against smallpox.
In 1799, the first vaccine institute was created in London and, in 1800, the British Navy began to adopt vaccination, also starting vaccination in America. In 1805, all French soldiers were vaccinated by order of Napoleon Bonaparte.
Unlike other scientific discoveries, the presentation of this vaccine did not give rise to much controversy, despite the fact that of some caricatures and statements against the results presented by Edward Jenner appearing. Everyone in general, both scientists and the population, understood the importance of this vaccine. From the beginning of the 19th century, there were large campaigns for antiviral vaccination, institutions were established for the spread of vaccination and the European population increased.
However, even in the eighteenth century, given the huge recognition of this vaccine, it was found that it was difficult to distribute it in order to reach the majority of the population. Charles IV (1748-1819), who at that time was king of Spain, devised an alternative to circumvent this problem by having 22 orphans vaccinated. The orphans later travelled to different regions and, using the blood of the immunized children, new vaccines were created for the local population.

Initially, doctors administered the vaccine with a forked needle that carried the bovine pathogen. Later, with the invention of the syringe, administration of the vaccine became easier.
In 1959, the World Health Organization (WHO) launched a worldwide campaign for the eradication of smallpox, which was considered the first disease eradicated by man through vaccination. In 1980, the WHO announced that this disease had been eradicated. The last reported cases were in Sudan, in 1977, and in a laboratory accident, in 1978. The last epidemic took place in Yugoslavia in 1972.
For 10,000 years, the smallpox virus has inhabited the Earth and caused millions of victims, an estimated 300 to 500 million in the 20th century alone. Although the smallpox vaccine prevented many deaths, it also saved millions of people from being left with scars and deformities for the rest of their lives.
Only 90 years later, at the end of the 19th century, Louis Pasteur (1822-1895) would be remembered for having discovered another vaccine, this one against rabies. He was the first to design a vaccine according to a scientific process. In his numerous works, he described the role of microorganisms in the transmission of infections and proposed therapeutic means of preventing these diseases, with varied processes to mitigate virulence.

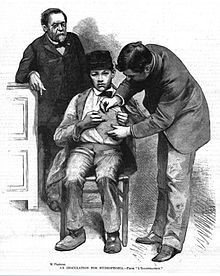
The infectious disease caused by the virus of the Lyssavirus genus entered and multiplied in the nervous system, expanding to the salivary glands. Thus, humans who were bitten by rabid dogs were infected with this disease. In 1885, Pasteur first applied the rabies vaccine to an eight-year-old child, Joseph Meister, who had been bitten by a rabid dog, using spinal cord extracts from a dog with the disease. Joseph Meister was the first person to survive the disease.
In 1879, Louis Pasteur discovered Bacillusanthracis and in 1881, together with his assistant Charles Chamberland, created and tried a carbuncle vaccine.
In 1887, Pasteur founded the Institute with his name in Paris, being its first director. Inaugurated the following year, the Pasteur Institute aimed to research biological, microbiological and in-depth studies on vaccines. The Pasteur Institute quickly gained great prestige, both nationally and internationally.

Over the years, the Pasteur Institute has been an international reference, with intense work in microbiological research that has led to important results in the control of some infectious diseases such as diphtheria, tetanus, tuberculosis, polio, influenza, yellow fever, and the plague. The AIDS virus (HIV) was isolated for the first time in the laboratories of the Pasteur Institute in 1983.
Thanks to the French and German schools, vaccination has made remarkable progress. The end of the 19th century and the beginning of the 20th century represented a major step forward, both with regard to the discovery of numerous bacilli, like Robert Koch (1843-1910), who discovered in 1882 the tubercle bacillus, or the discovery by Nicolaier in 1885 (the tetanus bacillus). As a result, vaccines against infectious diseases such as tuberculosis, diphtheria, tetanus and yellow fever were developed. After the Second World War, vaccines against polio, measles, mumps and rubella were created.

Vaccines in Portugal
After the discovery of the smallpox vaccine by Edward Jenner in 1798, the Portuguese doctor Manuel Joaquim Henriques de Paiva (1752-1829) published, in 1801, the work “Preservativo das Bexigas e dos Terriveis estragos ou Historia da Origem e Descobrimento da Vaccina, dos seus Effeitos ou Symptomas, e do Methodo de Fazer a Vaccinação & c.” (“Preservative of bladders and terrible damage or History of the Origin and Discovery of Vaccine, its Effects or Symptoms, and the Method of Vaccination & c.”).
In 1803, a translation of Edward Jenner's work was published with the title “Indagação sobre as causas, e effeitos das bexigas de vaccamolestia descoberta em alguns condados occidentaes de Inglaterra, particularmente na comarca de Gloucester, e conhecida pelo nome de vaccina” (Inquiry about the causes and effects of vaccollolysis bladders discovered in some western counties of England, particularly in Gloucester, and known by the name of vaccine)
.

In order to publicize Jenner's vaccine and apply smallpox vaccination, the Vaccinic Institution was founded in Portugal in 1812 at the Royal Academy of Sciences in Lisbon, thanks to the great encouragement given by Bernardino António Gomes (1768-1823). Five years after this date, it was found that in Portugal around 20,000 people had already been vaccinated, but there was a decline in vaccinations after the first two decades of the 19th century.

However, the great majority of Portuguese social classes recognized the importance of vaccination, which protected the population from the disease, decreased the mortality rate, and increased the average life expectancy. The people believed that the process should be universal and free.
As well as on a planetary scale, in Portugal, Pasteur's discoveries were also accepted in an exemplary way. In 1882, a Microbiology Office was founded in our country at the Faculty of Medicine of the University of Coimbra with the objective of carrying out tests of private and public interest and to be a centre of dissemination and practice of Pasteur's science.
In the following year, the Bacteriological Institute of Lisbon was founded which, in 1895, after having been moved from S. José Hospital, adopted the name of Royal Bacteriological Institute of Lisbon. In 1899, it was given its own facilities and adopted the name Câmara Pestana Royal Bacteriological Institute, in honour of its great promoter (Luís da Câmara Pestana, 1863-1899), who had died that year at the time of the plague epidemic in Porto.


The purpose of this Institute was the preparation of antitoxic serums for the treatment of diphtheria and tetanus, anti-rabies vaccination, deal with topics and research of general interest in microbiology and the preparation of vaccines, so that the cost of importing them was reduced.
Despite the Portuguese legislation referring to the mandatory nature of some vaccines, such as in 1894 regarding the smallpox vaccine and in 1962, the tetanus and anti-diphtheria vaccine, administered at the entrance of primary school and in secondary school, it was only in November 1965 that Portugal started a National Vaccination Programme (PNV), which consisted of providing the entire population with a set of vaccines in an appropriate manner, organized and in accordance with several previously established criteria. This procedure was initiated with the polio vaccine, denoting the interest the Portuguese population had in vaccination.
That year, the Individual Health Bulletin was implemented, where vaccines and the respective dates were registered. The tuberculosis vaccine was included in the vaccination programme.


In the following decades, several vaccines were included in the PNV, such as:
- 1973/1974 - Measles vaccine (VAS);
- 1987 - Vaccines against mumps and rubella administered together with measles;
- 1999 - Hepatitis B and Haemophilusinfluenzae type b;
- 2006 - Vaccine against meningococcus C;
- 2008 - Vaccine against the human papilloma virus (HPV);
- 2015 - The 13-valent conjugate vaccine against Streptococcus Pneumoniae infections (Pn13).
In 1977, smallpox vaccine was no longer mandatory due to the eradication of the disease. Polio is believed to be the next disease to be eradicated.
According to WHO data, between 2 and 3 million deaths are prevented every year due to vaccination against diphtheria, tetanus, whooping cough and measles.
In the current phase in which we are living, when the world is carrying out an authentic “marathon” to have access to a vaccine against Covid-19, which has already killed around 1.2 million people worldwide, it is important to recall the importance of the discovery of the first smallpox vaccine, which between 1896 and the late 1970s killed more than 300 million people, and was responsible for its eradication. Its discovery was a landmark for the health of humanity.
Although there are currently more than 50 vaccines for different diseases and in the last half century several vaccination awareness campaigns have been carried out, both health professionals and health authorities are aware that there is still much to do, because there is a need to create new vaccines for the diseases that have recently emerged, as well as for some old diseases for which there is still no prevention.
Infectious diseases are normally communicable diseases, which are caused by an external agent such as a virus, a bacterium or a parasite. On the other hand, vaccines are drugs that prevent infectious diseases. This medicine consists of a substance that is chemically similar or derived from an infectious agent that causes a specific disease. That is, vaccines are responsible for preparing the body to fight infectious diseases, stimulating the immune system after recognizing the invading agent, producing antibodies and providing the elimination of the pathogen. The vaccine will generate immunity, that is, protection in the body against infectious diseases. The vaccine is safe, efficient and an important ally in controlling, fighting and eliminating diseases, preventing painful treatments and protecting not only the recipient, but the community as a whole.
We all know that group immunity is essential and that human beings are not the only species to use the collective immunization method, ants also invest on the so-called “group immunization”. If one ant is infected with a fungus, the others "lick" the infected insect to spread the infection throughout the colony, making them all immune to the fungus in question.
Referências consultadas:
- EXHIBITION CYCLE. Health, Pharmacy and Society Topics. Accessed on 14/11/2020
- History. Accessed on 14/11/2020
https://webpages.ciencias.ulisboa.pt/~mcgomes/vacinacao/historia/index.html
- Vaccines that changed history. Accessed on 14/11/2020
https://visao.sapo.pt/atualidade/sociedade/2020-08-29-as-vacinas-que-mudaram-a-historia/
Lurdes Barata
Library and Information Centre
Editorial Team


