He catches our attention easily when we read his writings on his personal pages, or his articles in the Observador newspaper. He is a doctor with all his soul and has a mission, which is to take care of others. It is not in vain that he quotes Chekhov, his medical colleague, because he treads his path with the same life premise: "His legitimate wife is Medicine and his lover is Literature".
I don't think I ever said it publicly and I apologise for it: I love being a doctor, I love being a doctor at the National Health Service and I love being a doctor at Santa Maria Hospital (my house, it always has been, it will always be).
Of all the photographic memories of the past 11 months, I keep this one, from the first wave (still at the ward), with affection.
For all patients have given us and for all that this hospital has given us, I believe I can speak for almost all: we can all fall, but those on this side support your fall and will fall with you.
We are here, we will always be here until the last heart stops beating and, finally, silence covers a giant that will always insist on getting bigger and bigger.
This has been the case since 1953. It will be until the end.
Solid. - Miguel Esperança Martins
Between hectic schedules and the weariness that his eyes do not reflect, he reserves one of his few times off to give me this interview. It is Sunday morning, lunch is postponed so that he can give me some of his little time. Then he will set aside a few hours for his girlfriend Sofia, who is also a doctor, and at 8 pm he will be entering the emergency room for another long shift where he will try to do his best to keep alive Covid-19 patients who are naturally clinically unstable.
Miguel Maria Esperança Martins is an offspring of the Lisbon Academic Medical Centre (CAML). He has stopped at all the key pit stops of a path that will take him to intellectual wealth and greater human development.

From the year 10/16 of the Faculty of Medicine of the University of Lisbon, he left CAML for just one year to do the common year internship at Beatriz Ângelo Hospital, soon returning to Santa Maria Hospital, where he is currently completing his 3rd internship year in Oncology. In January 2021, he started conducting research at the João Lobo Antunes Institute of Molecular Medicine (iMM), with Sérgio Dias (Professor and Principal Investigator at iMM) and Luís Costa (Professor, Director of the Oncology Service of the HSM and iMM Principal Investigator). His research focuses on sarcomas, rare and less common tumours, which affect bone and soft tissue. He mentions Luís Costa to justify the importance of research in his life "in life, our greatest treasure is intellectual curiosity".
I wonder how Dr Miguel finds the time to do so many things. Where does his thirst to absorb more knowledge come from? Nothing in life has happened to him by chance, or without meticulous work. Still at the Faculty, he joined GAPIC to conduct his first scientific research projects. It was there that he learned to reconcile several tasks. In those days, he also took on the role of Anatomy and Neuroanatomy junior assistant.
Long before becoming a doctor, Miguel, born in São Sebastião da Pedreira, and the son of a lawyer (father) and a doctor (mother), was curious about many things. In his journey that would certainly be promising, he saw himself as a detective. He always loved to read in order to reach new worlds. His parents passed on to him the matrix of rigour and reconciliation between the World and Humankind. Created and formed by Jesuits, he speaks of his Faculty and São João de Brito school, where he studied until the end, with the same gratitude. “Educated to serve, that's what I was, and I am what I am”. He doesn't overdo the words, nor the emphasis he gives them.
He uses words almost like a child who plays freely and creates a thousand plots. We shall look into this other passion later on.
He believed that he was born serve and that he would be an investigative detective in the future. This is how his path started. Mix of concepts? No, it's all in the same bag. The first major topic to which he devoted his curiosity, in year 11 of schooling, was to understand the therapeutic usefulness of stem cells. At that time, he felt the ideas boiling in his head, questioned science, and explored the basis of his Catholic-based convictions. He describes the long conversation he had in the library of the former headquarters of the Brotéria magazine with one of the great mentors of his thought and character, Father and Professor Luis Archer. A scholar of Molecular Genetics, Humanities, Philosophy and Theology, he entered the Society of Jesus and was later ordained Priest.
When I ask him to explain how Science can cohabit with God the Creator, he smiles and calmly states that he is tolerant of all the codes and expressions of others. However, for him “the cellular, molecular, genetics complexity and epigenetics in all its changes are not the result of chance. What gives science more flavour is the human touch, touched by the divine”.
Having discarded becoming a professional detective, he decided he would be a cell detective and that is how research accompanied his development.
Like Alberto Caeiro, Miguel Esperança Martins also lets “all the little things amaze him”. Creating new questions and filling interstices was the mission of those who wanted to “unveil the veil of ignorance” with new clues or reasons.
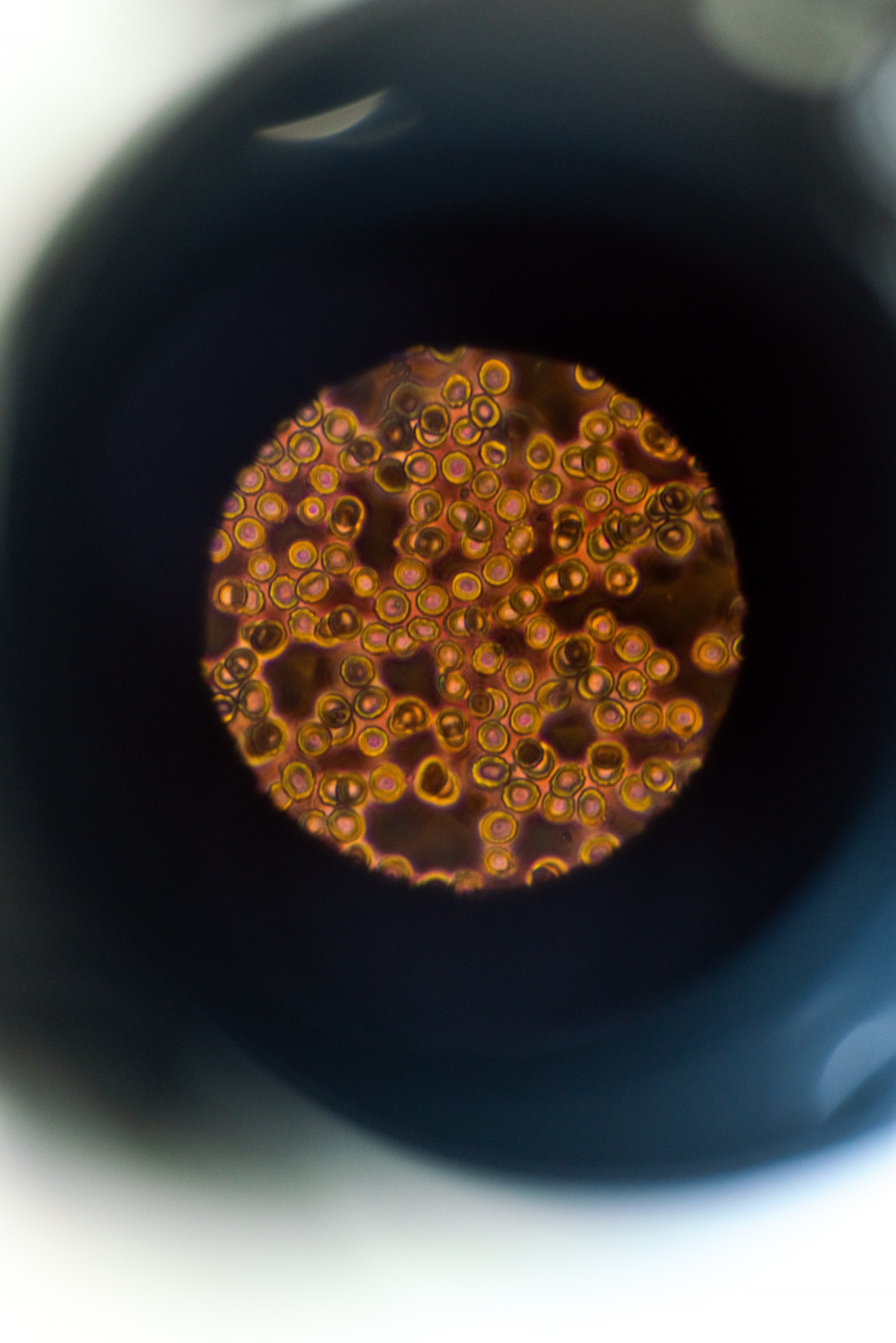
Can just a school shape someone's path like this? Certainly not. In addition to his parents, there were also his grandparents. The grandparents who have already passed away left him a rich heritage, the pleasure of being a reasonable storyteller, influenced by his paternal grandfather (lawyer), and the ethics and rigour of his maternal grandfather (internist). It was in the sum of what he received and the affections that he never lacked that he found the true influence in life and his great friendships in life: his parents, grandparents and Sofia.
Caring for and serving others is the role that he best plays and can do so in countless ways. When he travels and reflects on what he sees and who he sees, when he speaks other languages, or when he enters his hospital every day, the Lisbon University Hospital Centre, and goes to the hospital to treat patients who are infected with SARS-CoV-2.
Before starting his current 3rd internship in Oncology, Miguel Esperança Martins did two internships in London, one in Colorectal Surgery at St George’s Hospital, and another one in Oesophagus-Gastro-Duodenal Surgery at Imperial College (St Mary’s Hospital); in between he also did an internship in Cardiology in Rio de Janeiro.
What makes him go every day, is to enter the world of others, look at them in depth and feel how he can care for them, improve their destiny, or hold on to life.
Life is what Miguel Esperança Martins offers every day.
Being in Oncology, how do you end up in an area with covid-19 patients?
Miguel Esperança Martins: The Oncology internship includes a 21-month internship in Internal Medicine. I was precisely in that period with a person to whom I owe a lot and who taught me a lot, Dr Patricia Howell Monteiro, from Medicine 2C. At that time, we were faced with the challenge of treating patients newly diagnosed with SARS- CoV-2. Dr Patrícia brought the team together and we made the same commitment. It was like that. Between March and September 2020, I completed part of my internship in Internal Medicine, working permanently in isolation and hospitalisation units for patients with SARS-CoV-2 infection. I also completed part of my internship in the Intensive Care Unit, from October to December, in units dedicated to COVID-19 patients. I returned to my Oncology Service in January, but given the worsening of the situation in Portugal and the pressure that was placed on the hospital centre, it was necessary to mobilize an oncology intern in February to support wards full of new COVID-19 patients. I am currently part of the infectious disease service team in sector C (headed by Dr Armando Braz and Dr Maria João Gomes) and I support 24 patients with SARS-CoV-2 infection. So, my journey started in March last year and continues in February this year.

How does one feel when faced with such a scenario?
Miguel Esperança Martins: It was a mixture of feelings. I felt that I was being called to do what I was educated for, and, above all, to serve. When we realize that we are needed, we always feel imbued with a spirit of mission and it was this same spirit that filled me when it started. Then I also felt some fear, because, at the time, we dealt with an agent about which we knew very little. We had a relatively inaccurate and vague idea based on reports from Wuhan, but the different stages of the natural history of the disease were relatively poorly characterized. The catastrophic potential of this new agent was unknown, the type of tissue or organic tropism that the virus could present had been sparsely characterized, and despite all the protection material, the transmissibility had not been properly studied. Still, I felt enthusiastic, because I had the opportunity and the privilege to deal with something that, in the last decades, entire generations of doctors had not dealt with, a new pathology, entirely to be explored. The possibility of dealing with a pandemic is intellectually very stimulating. I seriously believe that in my future career, I will not have the opportunity to deal with a completely unknown agent and an absolutely unexplored illness. Watching the explosion of knowledge and scientific progress, being part of this process, integrating a global community that struggles to understand the mechanisms of the disease and proposing potential therapeutic targets is a very stimulating opportunity.
How are the routines of a doctor who treats covid patients?
Miguel Esperança Martins: When we enter the hospital, we always start with a small patient discussion meeting. A complete and extensive review of last night's patients’ conditions is always carried out and the main complications are discussed. There are certain aspects in which we focus more particularly, such as the patients’ ventilatory pattern, that is, the degree of ventilatory comfort manifested by the ability to tolerate efforts, respiratory rate, use of accessory breathing muscles, bluish colour of the skin and mucous membranes. After this review, we define which patients we will approach first and who need to be observed as soon as we enter. We then move on to the disinfecting and equipment ritual. We wash our hands, wear the suit, there are those who prefer to wear it in full, or just one of the gowns, followed by the placement of the foot protection, the cap, the full face mask when necessary, then the eye protection, consisting of glasses or shield, and, finally, the gloves. I always wear two pairs of gloves. We collect all the necessary material for the first patient we are going to see. If later we need some other instrument or material, we will ask for what we need inside, the red zone. Having seen the most serious cases, I always make it a habit to take a quick tour around all the patients to see how they are.
And how do you deal emotionally with patients who are in more severe medical conditions?
Miguel Esperança Martins: This is when what makes me a doctor stands out. If I have a patient who has a high probability of acute respiratory failure in the short term, it is clear that I have to act with another degree of readiness and precision. I have to explain quickly, albeit calmly, to the patient, very directly and clearly, what will happen. And what I explain, when it is necessary and the patient has the ability to fully understand, is that we will need to sedate him and insert an orotracheal tube, stressing that the procedure will be painless and absolutely crucial for him to overcome the most critical phase of his illness. A doctor can heat up inside alone, but he always does so in isolation. To the others, the doctor needs to show calm, tranquillity and safety.
What impressed me the most, due to its extraordinary emotional and human density, were the last phone calls before an intubation. I have witnessed some and there are voices and sounds that will always echo in my mind. I've seen several, with varied tones and content. I will write an extensive chronicle reporting this. I don't forget the last call from a young patient to his father. It was extraordinarily brief, given the patient's dyspnoea and fatigue, but all the affection and love poured in half a dozen words. After explaining to the father the seriousness of the clinical situation and then passing the phone to the patient, the only thing he was able to say was "see you soon". Have you any idea of what is like to say goodbye to your father in this way? How counter-natured is this? There is another case when I was the one who made the connection to the patient's wife and children. I explained the clinical gravity of the situation to the patient's wife and passed the phone on to the patient who, between two or three short sentences, found the strength to cry and express a message for eternity to his family. Interestingly, two weeks later, the patient returned from Intensive Care and when I went to the Internal Medicine service, I received him back. Upon entering the room, the patient looked at me briefly and, although he was still affected by hyperkinetic delirium, pointed and frantically repeated "You told me it would be okay". I don't forget that. These moments, more than being the result pf duty and medical ethics, are moments of pure humanity, of union with someone like us at a time of maximum fragility and fear. Cases like this shape our character and endow everyone with humbleness and huge respect for what we do not control at all. Throughout this year, even if I am not an intensivist, I have seen and experienced incredible situations. I believe that if I interviewed my fellow internists, anaesthetists and intensivists, who are the ones who are most often with the patients at these occasions, I would certainly have material for several textbooks. They are human beings and History was made, is made and will be made out of human beings.
But as in any human story, it sometimes goes wrong...
Miguel Esperança Martins: Yes, of course...

So, as doctors, you never break down in public...
Miguel Esperança Martins: Ideally, no. In practice, it is virtually impossible for it not to happen, because the patients who surround us observe us, they know that on this side there are other human beings wearing gowns, gloves and laryngoscopes. And all of us, as carbon shells populated by emotions, tend to be affected emotionally, of course. At the moment, we can block emotions and remain rationally intact. We try to remain neutral and rational, but we always end up reflecting (voluntarily or involuntarily) about what life presents us with. Whether we like it or not. We all have our cemetery, we are all assailed by certain ideas and reflections. Always!
Do you ever feel afraid because you are so close to this virus?
Miguel Esperança Martins: The fear is always there. To deny it would be unreal. In my case, my main fear is to inadvertently infect those closest to me, creating a situation as catastrophic as those I deal with in the hospital. The moment we have a patient before us, the concern for us, as a general rule, goes away. We are shaped to help others, to serve and, as such, our survival instinct is put at the service of others. Our main concern is to save and preserve the life of the person we are dealing with and who places himself in our hands. Do I care about myself in general terms? Yes, in general, but my main concern is the patient in front of me, my family and my girlfriend. I think that neither I nor my colleagues are very concerned with what might happen to us. Of course, we are careful. We go in properly equipped, but our concern, and I think it is almost universal and transversal to everyone I worked with this year, is to save patients.
As a doctor in the midst of a calamity, can you say if the patients’ profile has changed over time?
Miguel Esperança Martins: These times have been different from the first wave, and different from the second wave, too. In other words, we have always had very serious, highly complex patients, because we are a tertiary hospital centre, the largest hospital in the country. As such, we receive patients with the entire spectrum of disease severity. What I have noticed is that in recent weeks, there has been a highest proportion of patients with moderate to severe illness. On the other hand, there is the finitude of human resources available to respond to this avalanche. We are practically the same people who have been here since March 2020. Of course, more people have since joined us. And here I talk about my reality and my hospital. The spirit of mutual assistance, from one service to the next, has been absolutely extraordinary. At the moment, I work in an isolation unit with 4 general surgery interns and 2 otorhinolaryngology interns, with surgical specialties, who do not usually deal with patients with acute respiratory pathology. They are doing their best to give the best possible response in this context. We have had an extraordinary capacity for unity! We strive, we do our best, we work for endless hours. We have been working at an extraordinary pace for a year. However, human resources are, in fact, finite and the calamity that has befallen the SNS has taken stratospheric proportions.
While praising the Internal Medicine (in particular “my” Medicine 2) and Infectious Diseases services, which have been able to open wards at astonishing speed, it is difficult to provide maximum quality care to so many patients at the same time. The same applies to the Intensive Care Service, which has made an extraordinary expansion, doubling the bed capacity in a few months. Another example is the “Covid ward”, the ER unit that we have out there. This is also a service where small miracles are performed. The emergency teams have been working at 200% or 300%, dealing with incredibly complex patients, working for endless periods in that space. They do the impossible until they are able to come up with more beds in the hospital structure. All CHULN professionals are here to respond to this situation. What I wrote last week reinforces what I tell you, this giant has been here since 1953 and will be here until the end.
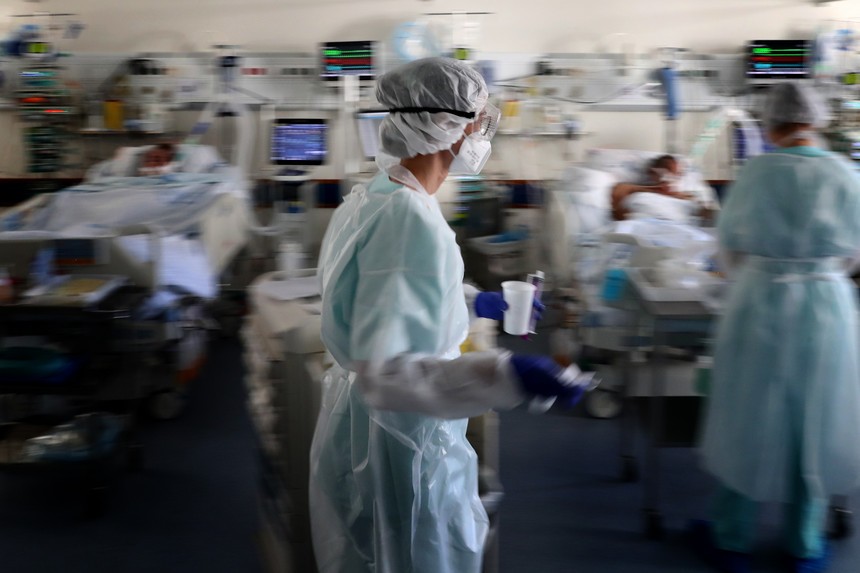
The feeling we have is that, in hospitals, you live in a war scenario…
Miguel Esperança Martins: Probably yes, but our goal is precisely to counter this perception. Of course, we are practicing catastrophe medicine, how can we deny it? Regardless of this scenario, the truth is that all professionals have made an extra effort not to show this to our patients. Look again at the case of the "Covid Unit". Despite the significant number of patients on non-invasive ventilation, or on very significant oxygen intake, the truth is that patients are awake, hear us, see us. We are well aware of the need not to show an image of chaos, disorganization or panic. We do not want to pass on the idea that we are making choices, when they are only made at the limit. Patients cannot have this image of health care, not only those who are in the Covid unit, but also those who are waiting, as well as those who are at home. The situation management message that must go through is the guarantee of possible tranquillity, even if it does not exist in full. War medicine shows us that there are choices and decisions that are made in extreme situations. If I said that this is not true, I would be lying. In the shifts I took, either in the central emergency room, in the Internal Medicine ward, or in the Intensive Care Unit, no patient has failed to be properly assisted and comforted regardless of the enormous pressure to which we are subjected.
What does a doctor feel when having to decide to save one life at the expense of another?
Miguel Esperança Martins: Fortunately from that point of view, from what I was told, everything has been guided by scientific rationality, however fair and realistic. Limit decisions in relation to patients are always taken as a team. There is a sharing and communion of positions among the persons that make up each team. If the patient is a candidate for additional organ support measures and needs to stay in an intensive care unit, it is always discussed with the Intensive Care Unit. Of course, at the end of the day, when all the adrenaline goes, when everything that immediately occupies our head fades and the dust settles, we think and reflect on the situations we deal with. This is normal. At the moment, those who lead Internal Medicine, Infectious Diseases or Intensive Care Medicine teams, certainly have a lot to think about. Usually after 30 or 40 hours of uninterrupted service. It is beautiful and important to respect that.
(long silence)
How will your head be when this pandemic goes away?
Miguel Esperança Martins: My head will be extraordinarily busy. We will all deal with the side effects of this pandemic. Me, specifically, in my Medical Oncology area. We have ensured the follow-up of all patients who are undergoing active systemic antineoplastic therapy. Here I must refer to the extraordinary management on the part of my advisor and director, Professor Isabel Fernandes (and also Dr Daniela Macedo). We will deal, however, with patients who will have a significant diagnostic and therapeutic delay. We will also pay attention to cardiovascular, endocrinological pathologies, and other ones. The entire National Health Service will have to deal with and endure all of this time distortion. The heads of all the doctors at this hospital will be particularly busy dealing with all of this. On the other hand, I believe that I will also be much more able to recognize and deal with extreme situations. Whether we like it or not, this gives us a lot of experience. I honestly hope that my mind is not occupied by this pandemic. Let us hope that these mutagenic processes of the virus do not prevent or diminish the achievements that the already approved and launched vaccines promise. I will also reflect on the harmful effects that this pandemic will have on the economic fabric of our country, with harmful consequences for all. Without exception.
In one of the articles for Observador, you wrote, and I quote: “Today we intubated and ventilated a young man. Few know how difficult it is to watch helplessly the marked and accelerated deterioration of the clinical condition of a patient on whom so much is invested as to therapeutic strategy. (…) They insist, in a defiant tone, on denying science and on basing political and ideological opinions and fanaticisms on a conceptual house of cards. They believe that science and politics are at the service of each other. I will be objective: None of that matters to me. I am not a politician. I serve the interests of those I care for. My ideology is Medicine”.
Was what has gone wrong due to bad political decisions? Has it been the excess of coexistence between people? Are decisions yet to be made?
Miguel Esperança Martins: I stick to my clinical practice. Out of the politically correct, I have always stated that I am here as a doctor and only as a doctor. It is a fact that the situation has worsened a lot, the figures are public. Hospital pressure has increased markedly. This is due to epidemiological factors and to factors intrinsic to the virus itself and its variants. I do not believe it is a stage for critical and accusatory assessments. I am not defending that one should not argue. I believe that, above all, one should discuss the matter in depth with those who have enough data and knowledge to do so. I will not give my opinion on this because I just talk about what I see and what I really know, which is clinical medicine. With regard to political analysis, I have no skills, nor the knowledge. I am not an epidemiologist nor a specialist in public health, I do not have the full statistical data. What I find most shocking regarding opinions in Portugal, is seeing and hearing a lot of people who never entered a COVID unit, who never saw a COVID patient, who never even entered a hospital where COVID patients are cared for, who do not have a medical degree, with no solid knowledge of applied statistics, with no epidemiological basis for issuing opinions and judgments about hospital praxis, giving their opinion with the pseudo-seriousness, credibility and equidistance they advocate. I am still waiting to see so many specialists with an apparent foreground appear in the emergency room, in an infirmary, in an intensive care unit. I do not talk about what I do not master. In life, we have to know how to put ourselves in our place. My place here is as a doctor. Even when I scribble my chronicles, I describe the human dimension of each reality, with the utmost scientific rigor. And that is it.

Shall we talk about the deniers?
Miguel Esperança Martins: It is another phenomenon that has amazed me. This is a country where Sisyphus and Nero reign. We clinicians are Sisyphus (a character in Greek mythology who was condemned to repeat the task of pushing a rock to the top of a mountain). That is, we push the rock permanently to the top of the mountain and always deal with another flood, another avalanche. They throw the rock down the mountain again, and we carry the rock up the mountain every day. And in a country where many Sisyphus (es) and Nero (s) coexist (Roman emperor known for his tyranny. There are historical currents that believe that it was he himself who ordered the great fire of Ancient Rome, to "clean" the city to his liking and to persecute Christians) they play the harp and sing while Rome burns. The message I want to leave is that it is essential that people realize who Nero is and who Sisyphus is. One just needs to pat attention.
Do you feel you will come out of this more experienced?
Miguel Esperança Martins: Undoubtedly. Experience is always enriching for people, amplifying the quality of their practice. There is a fabulous quote that I think is on the wall opposite the Mark Athias amphitheatre, which is by Rhazes, and talks about the importance of reading to prepare the doctors’ critical stance, although not fully. Practice is what makes us doctors. This experience prepares me as a doctor, to deal with a multitude of clinical situations that I had not yet dealt with and prepares me as a Man in relation to others, because people and extreme situations always end up shaping our character. There are things that my colleagues and I will never forget in 40 or 50 years. I became less optimistic, perhaps more realistic and cautious. Surely better prepared for contexts that a few years ago would have been unimaginable.
Was this pandemic a needed lesson for Humanity?
Miguel Esperança Martins: This is a good question that will force me to think... (long sigh). I would say that there are things that we must learn, particularly with regard to what we cannot control and how to deal with it. It renewed in everyone the old maxim that, alone, we may be able to go faster, but together we go further. We realize that together we are able to boost our human capital in its most different aspects in a completely different way. Perhaps it reminds the vast majority of people of the need to have empathy and respect for others. Some notions of fairness may also have surfaced. We have learned things but I think that lesson is too crude and harsh a term that presupposes that this disease has triumphed over what was the response capacity of a humanity that will triumph over it. It took and will take some of us, but it did not collectively triumph over humanity. Hope remains and will always remain.
Joana Sousa
Editorial Team


